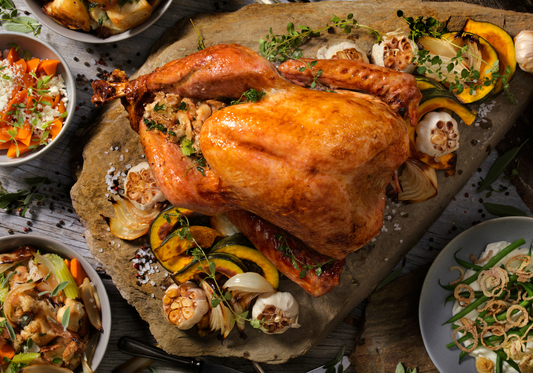
Low Histamine Holiday Turkey Recipe
It's turkey time! Whether it's Christmas, Thanksgiving or just your weekly Sunday roast, histamine intolerance can make dinner planning suck, a lot.So, it's a major win when you can find...
Low Histamine Holiday Turkey Recipe
It's turkey time! Whether it's Christmas, Thanksgiving or just your weekly Sunday roast, histamine intolerance can make dinner planning suck, a lot.So, it's a major win when you can find...

Low Histamine Turkey Stuffing Recipe (With Brea...
Are you ready to STUFF. YOUR. FACE... with my low histamine stuffing recipe, of course.Today, I've got a gluten-free, low histamine stuffing recipe that's made entirely from scratch, down to...
Low Histamine Turkey Stuffing Recipe (With Brea...
Are you ready to STUFF. YOUR. FACE... with my low histamine stuffing recipe, of course.Today, I've got a gluten-free, low histamine stuffing recipe that's made entirely from scratch, down to...

Low Histamine Pumpkin Mousse Dessert Recipe
Pumpkin is such a staple for the holidays!But pumpkin-flavored holiday favorites are generally loaded with ingredients that are a big no-no when it comes to histamine intolerance. So here, I...
Low Histamine Pumpkin Mousse Dessert Recipe
Pumpkin is such a staple for the holidays!But pumpkin-flavored holiday favorites are generally loaded with ingredients that are a big no-no when it comes to histamine intolerance. So here, I...

Low Histamine Cauliflower Rice Pudding Recipe
Who doesn't love a good low histamine dessert - especially when that means PUDDING!But along with the word dessert, usually come a lot of questions regarding health and nutrition: Should...
Low Histamine Cauliflower Rice Pudding Recipe
Who doesn't love a good low histamine dessert - especially when that means PUDDING!But along with the word dessert, usually come a lot of questions regarding health and nutrition: Should...

Low Histamine Ground Beef Tacos Recipe
It's time to turn your dinner table into a low histamine Mexican fiesta... in under 20 minutes!Tacos contain a million and one high histamine ingredients (1)...and, I bet you never thought...
Low Histamine Ground Beef Tacos Recipe
It's time to turn your dinner table into a low histamine Mexican fiesta... in under 20 minutes!Tacos contain a million and one high histamine ingredients (1)...and, I bet you never thought...

Is Histamine Causing Your Unwanted Symptoms?
Do you experience reactions to foods, even though you seem to be eating a healthy, natural diet?Do you have symptoms like digestive distress, skin rashes, headaches, anxiety or allergy-like symptoms?Well,...
Is Histamine Causing Your Unwanted Symptoms?
Do you experience reactions to foods, even though you seem to be eating a healthy, natural diet?Do you have symptoms like digestive distress, skin rashes, headaches, anxiety or allergy-like symptoms?Well,...

Heavy Metal Toxicity and Histamine Intolerance
What do heavy metals have to do with histamine intolerance?In our everyday lives, we’re exposed to a fair number of compounds that enter our body systems through the environment.In some...
Heavy Metal Toxicity and Histamine Intolerance
What do heavy metals have to do with histamine intolerance?In our everyday lives, we’re exposed to a fair number of compounds that enter our body systems through the environment.In some...

Maple Oatmeal Low Histamine Cookie Recipe
Are you hankering for some low histamine cookies? Boy oh boy have I got a surprise for you. And, being the Canadian that I am, this recipe obviously includes my...
Maple Oatmeal Low Histamine Cookie Recipe
Are you hankering for some low histamine cookies? Boy oh boy have I got a surprise for you. And, being the Canadian that I am, this recipe obviously includes my...

Histamine Intolerance and Your Brain: Sleep, Mo...
Are you wondering how histamine intolerance affects your brain? By now you’re likely aware of the effects of histamine on your overall health and how an excess of histamine is the...
Histamine Intolerance and Your Brain: Sleep, Mo...
Are you wondering how histamine intolerance affects your brain? By now you’re likely aware of the effects of histamine on your overall health and how an excess of histamine is the...

Trauma and Histamine Intolerance
Look online for that underlying cause of your histamine intolerance and you’re most likely to find a bunch of reasons that involve: The blocking of the histamine degrading enzyme, diamine...
Trauma and Histamine Intolerance
Look online for that underlying cause of your histamine intolerance and you’re most likely to find a bunch of reasons that involve: The blocking of the histamine degrading enzyme, diamine...

3 Tips to Prevent Hangovers
Do you experience hangovers? Then boy do we need to talk!Last week, I sent an email to some of my followers giving them an insider tip on how to cure...
3 Tips to Prevent Hangovers
Do you experience hangovers? Then boy do we need to talk!Last week, I sent an email to some of my followers giving them an insider tip on how to cure...

Low Histamine Cauliflower and Pomegranate Salad...
Are you ready for a sweet and savoury combo that will knock your socks off? Well this low histamine cauliflower and pomegranate salad packs a punch!This delicious smokey and crunchy...
Low Histamine Cauliflower and Pomegranate Salad...
Are you ready for a sweet and savoury combo that will knock your socks off? Well this low histamine cauliflower and pomegranate salad packs a punch!This delicious smokey and crunchy...

Creamy Coconut Chicken Low Histamine Soup Recipe
Looking for a delicious low histamine soup? Whether it’s soup soup season or summer time, everybody craves a delicious creamy soup now and again.But, for those with histamine intolerance, finding...
Creamy Coconut Chicken Low Histamine Soup Recipe
Looking for a delicious low histamine soup? Whether it’s soup soup season or summer time, everybody craves a delicious creamy soup now and again.But, for those with histamine intolerance, finding...

Why Histamine Intolerance Causes Headaches and ...
Are you wondering if a histamine intolerance could be linked to your headaches and migraines? By now you’re likely quite familiar with what histamine intolerance is and the symptoms it may...
Why Histamine Intolerance Causes Headaches and ...
Are you wondering if a histamine intolerance could be linked to your headaches and migraines? By now you’re likely quite familiar with what histamine intolerance is and the symptoms it may...

Is There a Test for Histamine Intolerance?
Is there a test for histamine intolerance?If you believe you are histamine intolerant and are looking for a histamine intolerance test, we need to talk.Histamine intolerance can be frustrating, as...
Is There a Test for Histamine Intolerance?
Is there a test for histamine intolerance?If you believe you are histamine intolerant and are looking for a histamine intolerance test, we need to talk.Histamine intolerance can be frustrating, as...

Nutrient Deficiencies with Histamine Intolerance
Could your low histamine diet be contributing to nutrient deficiencies?When it comes to managing histamine intolerance, surely nothing can be worse for you than eating foods packed with histamine, histamine...
Nutrient Deficiencies with Histamine Intolerance
Could your low histamine diet be contributing to nutrient deficiencies?When it comes to managing histamine intolerance, surely nothing can be worse for you than eating foods packed with histamine, histamine...

Histamine Intolerance: Medications to Avoid
Can’t get a grip on your histamine intolerance symptoms? Take a look at these common medications as a potential cause… In today’s world, it’s not uncommon to find someone that...
Histamine Intolerance: Medications to Avoid
Can’t get a grip on your histamine intolerance symptoms? Take a look at these common medications as a potential cause… In today’s world, it’s not uncommon to find someone that...

Crispy Roasted Low Histamine Chickpeas Recipe
Looking for a crunchy snack that's histamine safe? Here's an unbeatable low histamine chickpeas recipe for the win!Instead of heading to a questionable restaurant and having symptoms by the time...
Crispy Roasted Low Histamine Chickpeas Recipe
Looking for a crunchy snack that's histamine safe? Here's an unbeatable low histamine chickpeas recipe for the win!Instead of heading to a questionable restaurant and having symptoms by the time...

Honey Garlic Low Histamine Roast Chicken Recipe
If all you're craving is a low histamine chicken recipe, then I've got just the one for you!Sweet, savory, succulent, crispy....everything you could wish for all wrapped up into one...
Honey Garlic Low Histamine Roast Chicken Recipe
If all you're craving is a low histamine chicken recipe, then I've got just the one for you!Sweet, savory, succulent, crispy....everything you could wish for all wrapped up into one...

Stewed Apples Recipe for Histamine Intolerance
There's some truth to the saying 'an apple a day keeps the doctor away'... however, it may not be for the reasons you assume. Today, I'd like to share some...
Stewed Apples Recipe for Histamine Intolerance
There's some truth to the saying 'an apple a day keeps the doctor away'... however, it may not be for the reasons you assume. Today, I'd like to share some...

How I Solved My Histamine Intolerance
If you’re histamine intolerant, you’ll be well-experienced in the struggles and difficulties of searching for a histamine intolerance treatment.You have to struggle with constantly trying to manage and worry about...
How I Solved My Histamine Intolerance
If you’re histamine intolerant, you’ll be well-experienced in the struggles and difficulties of searching for a histamine intolerance treatment.You have to struggle with constantly trying to manage and worry about...

Histamine and Stress: Why Stress is Toxic for H...
Did you know that there is a close relationship between histamine intolerance and stress?In fact, the levels of stress and histamine release impact one-another dramatically.And - your brain may be...
Histamine and Stress: Why Stress is Toxic for H...
Did you know that there is a close relationship between histamine intolerance and stress?In fact, the levels of stress and histamine release impact one-another dramatically.And - your brain may be...

Herby Low Histamine Salad Dressing Recipe
Are you looking for a delicious low histamine salad dressing recipe? Let's face it, most salad dressing recipes, even if they're homemade, contain ingredients that are pretty unfriendly to those...
Herby Low Histamine Salad Dressing Recipe
Are you looking for a delicious low histamine salad dressing recipe? Let's face it, most salad dressing recipes, even if they're homemade, contain ingredients that are pretty unfriendly to those...

The Antihistamine Diet: Antihistamine Foods Lis...
What if antihistamine foods could change your body and improve your symptoms for good?What if an antihistamine diet could improve your digestion, your skin, change your sleeping patterns, eliminate pain,...
The Antihistamine Diet: Antihistamine Foods Lis...
What if antihistamine foods could change your body and improve your symptoms for good?What if an antihistamine diet could improve your digestion, your skin, change your sleeping patterns, eliminate pain,...


